Research Highlights
Honorable Mention – OVT, AAOS 2026
- Technique for Safe Harvesting of Bone Marrow Aspirate Concentrate During Hip Arthroscopy
1st Place- Kilfoyle Award for Best Original Scientific Paper, EOS 2025
- Characterization of Human Bone Marrow Aspirate Concentrate-Derived Mesenchymal Stem Cells and the Effect of Commonly Used Clinical Drugs on Their Viability and Proliferation
2024 JBJS Essential Surgical Techniques Subspecialty Procedures Award, JBJS 2025
- Puncture Capsulotomy Technique During Hip Arthroscopy
John D. Kelly IV, MD Travel Grant Award, EOA 2025
- All-Arthroscopic Capsular Autograft Hip Labral Reconstruction: Minimum 5-Year Functional Outcomes.
Recognized as one of the top submissions in its category (Biologics), AANA 2025
- Five-Year Outcomes Following Acetabular Labral Repair with Bone marrow Aspirate Concentrate
Excellence in Research Award Finalist, AOSSM 2025
- Six-Month Functional Scores Predict 5-Year Outcomes after Hip Arthroscopy for Symptomatic Acetabular Labral Tears
Top Poster Submission in Biologics, AANA 2025
- Five-Year Outcomes Following Acetabular Labral Repair with Bone marrow Aspirate Concentrate.
Special Recognition: AOSSM Specialty Day Symposium, AAOS Annual Meeting, 2025
- Global Acetabular Retroversion Is Associated with Increased Risk of Conversion to Total Hip Arthroplasty after Primary Hip Arthroscopy and Greater Chondrolabral Junction Breakdown: A Propensity- Matched Analysis with Minimum 8-Year Follow-up.
Special Recognition: AOSSM Specialty Day Symposium, AAOS Annual Meeting, 2025
- Hip Arthroscopy Patients Experiencing Greater Neighborhood-Level Socioeconomic Disadvantage are More Likely to Achieve Minimal Clinically Important Diff erences in Functional Outcomes at 1-Year Follow-up.
O’Donoghue Research Award Winner, AOSSM Annual Meeting, 2024
- Hip Arthroscopy Versus Physical Therapy for the Treatment of Symptomatic Acetabular Labral Tears in Patients Older Than 40 Years: A 2-Year Report of A Randomized Controlled Trial
Best Sports Medicine Poster Presentation, MSOS Annual Meeting, 2024
- The role of chondrolabral junction breakdown on functional outcomes following hip arthroscopy at minimum two-year follow-up.
Best Clinical Paper, Orthopaedic Summit, 2023
Chondral Flap: Patients with Worse Chondral Damage Report Better Two-Year Functional Outcomes After Treatment with Bone Marrow Aspirate Concentrate During Acetabular Labral Repair.
Areas of Study, 2025
- Caprine Study
- Histological staining
- Electron Microscopy
- Polarized Light Microscopy
- Bone Marrow Aspirate Concentrate (BMAC)
- PROMs
- Randomized controlled trial: BMAC vs no BMAC (actively enrolling)
- Cell Analysis
- Retrospective Study of Labral Repair with Chondrolabral preservation (>10 years, >5 years, >2 years)
- Randomized Controlled Trial in Hip Arthroscopy vs. Physical Therapy in Patients Over 40 (2-year follow-up)
- Laser Doppler to measure blood flow to the chondrolabral junction
- Orthobiologics
- Abductor Tendon
Hip Joint: Recent Significant Publications
Gluteal Tendon Repair Using an Endoscopic Transosseous Equivalent Double Row Repair Technique, JBJS Essential Surgical Techniques
Mun JS, Gillinov SM, Lee JS, Martin SD. Gluteal Tendon Repair Using an Endoscopic Transosseous Equivalent Double Row Repair Technique. JBJS Essential Surgical Techniques. July-September 2025; 15 (3): e24.00025 https://doi.org/10.2106/JBJS.ST.24.00025
Surgeon-Driven Variation in the Cost of Hip Arthroscopy for Labral Pathology: A Time-Driven Activity-Based Costing Analysis, Am J Sports Med
Background: Amid mounting pressure to reduce health care spending, strategies for identifying and eliminating unwarranted variation in costs have garnered significant attention. Previous studies have characterized intersurgeon variation in costs for common orthopaedic procedures, but such variation remains unexplored in the context of hip arthroscopic surgery.
Purpose: To (1) characterize variation in the cost of hip arthroscopic surgery between surgeons using time-driven activity-based costing (TDABC) and (2) identify patient characteristics, intraoperative findings, and operative procedures underlying such intersurgeon variation in costs.
Study design: Cohort study; Level of evidence, 3.
Methods: Employing TDABC, the authors determined the intraoperative cost of 890 outpatient hip arthroscopic surgery cases performed by 5 surgeons at 4 surgery centers from 2015 to 2022. All costs were calculated in United States dollars. Costs were normalized to protect the confidentiality of internal hospital cost data. Surgeon-specific mean costs were calculated with and without adjustment for patient characteristics, surgical personnel, operative factors, and surgery center. Finally, to elucidate the sources of surgeon-driven cost variation, the authors estimated the proportion of variation attributable to different cost subcategories, including labor, implant/allograft, and other supply costs.
Results: The intraoperative cost per patient ranged from 38.2 to 212.8 normalized cost units (mean, 100.0 ± 26.5), with a 1.6-fold variation in the mean cost between the highest and lowest cost surgeons. Operating surgeon alone explained 53.4% of the observed variation in costs. Controlling for case-specific features significantly improved the explanatory power to 91.8% (P < .001), but the adjusted variation in costs between surgeons remained essentially unchanged (decreased by <3%). Each of the 5 surgeons generated costs that deviated significantly from those predicted based on case-specific factors, with mean surgeon deviations ranging from -5.0% to 21.8% (P < .001 for all). Drivers of cost variation differed substantially between surgeons but generally stemmed from labor or other supply costs rather than implant/allograft costs.
Conclusion: The cost of outpatient hip arthroscopic surgery varied widely between surgeons; the cause of this deviation was multifactorial and surgeon specific. While within-surgeon cost variation was effectively explained by patient and operative characteristics, most between-surgeon variability remained unexplained by observable factors. These insights may support individual surgeons in cost reduction efforts and, more importantly, may enable the alignment of reimbursement rates with costs.
Dean MC, Cherian NJ, Beck da Silva Etges AP, Dowley KS, Torabian KA, LaPorte ZL, Martin SD. Surgeon-Driven Variation in the Cost of Hip Arthroscopy for Labral Pathology: A Time-Driven Activity-Based Costing Analysis. Am J Sports Med. 2025 Jun 5;53(8):1869–1877. http://doi.org/10.1177/03635465251341463 PMID: 40474356
Five-Year Functional Outcomes Following Acetabular Labral Repair with versus without Bone Marrow Aspirate Concentrate, JBJS
Background: Bone marrow aspirate concentrate (BMAC) augmentation at the time of hip arthroscopy is a potential solution to improve functional outcomes in patients with cartilage damage concomitant with acetabular labral tearing; however, follow-up functional scores to date have not exceeded 24 months. Therefore, the present study compares minimum 5-year outcomes in patients treated with or without BMAC augmentation to address chondral damage during arthroscopic labral repair.
Methods: This was a prospective cohort study analyzing patients who underwent acetabular labral repair performed by a single surgeon. Patients were stratified into either the BMAC cohort or the control cohort depending on whether BMAC was utilized in conjunction with arthroscopic labral repair. Demographic and intraoperative variables, including chondrolabral junction breakdown and articular cartilage damage, were compared between cohorts, as were patient-reported outcome measures (PROMs) at enrollment and at 3, 6, 12, 24, and 60 months postoperatively.
Results: Eighty-one hips were included for analysis: 39 (38 patients) in the BMAC cohort and 42 (39 patients) in the control cohort. Univariate analyses demonstrated similar baseline characteristics between groups, including body mass index, Tönnis angle, lateral center-edge angle (LCEA), and alpha angle (p > 0.05 for each). Patients treated with BMAC and patients in the control group reported similar PROMs between enrollment and the 12-month follow-up. By the 24-month follow-up, patients treated with BMAC reported significantly higher scores for the modified Harris hip score (mHHS) (p = 0.004), the International Hip Outcome Tool-33 (iHOT-33) (p = 0.012), and the Hip Outcome Score-Activities of Daily Living (HOS-ADL) (p = 0.008). This trend persisted over time, with the BMAC cohort demonstrating significantly higher scores for the mHHS (p < 0.001), iHOT-33 (p = 0.006), and the Hip Outcome Score-Sports Subscale (HOS-SS) (p = 0.012) at 60 months.
Conclusions: Patients undergoing acetabular labral repair with BMAC augmentation reported significantly greater functional improvements compared with patients undergoing repair without BMAC. These differences generally did not become significant until 24 months after surgery, at which point they increased in magnitude until the 60-month follow-up. These findings, the first intermediate-term outcomes reported following hip arthroscopy with BMAC, therefore suggest favorable benefit at an extended follow-up.
Martin SD, Dowley KS, Siddiq BS, Gillinov SM, Lee JS, Cherian NJ, Eberlin CT, Kucharik MP, Dean MC. Five-Year Functional Outcomes Following Acetabular Labral Repair with versus without Bone Marrow Aspirate Concentrate. J Bone Joint Surg Am. 2025 May 30;107(14): 1570-1578. https://doi.org/10.2106/JBJS.24.00602 PMID: 40446023 2025 May 30. Online Ahead of Print.
Association Between Global Overcoverage and Long-term Survivorship, Chondrolabral Junction Breakdown, and Reduced Joint Space Width: Minimum 8-Year Follow-up, Am J Sports Med
Background: Although previous literature has established the association between femoroacetabular impingement and progressive hip osteoarthritis, there exists a paucity of studies investigating the effects of global acetabular overcoverage on chondral wear and long-term outcomes.
Purpose: To compare baseline joint space width (JSW), intraoperative findings, long-term total hip arthroplasty (THA)-free survivorship, patient-reported outcome measures (PROMs), pain levels, and patient satisfaction in patients who underwent hip arthroscopy with global overcoverage (GO) to a matched-control (MC) cohort.
Study design: Cohort study; Level of evidence, 3.
Methods: In this retrospective analysis, the authors queried patients who underwent hip arthroscopy for acetabular labral tears secondary to femoroacetabular impingement. Patients with complete PROMs at a minimum 8-year follow-up, the presence of coxa profunda as indicated by an acetabular wall projecting medial to the ilioischial line, and a lateral center-edge angle >40° were matched 1:1 by sex, age, body mass index, Tönnis grade, and labral treatment to a MC cohort of patients who had normal acetabular coverage. Baseline radiographic and intraoperative findings were compared between cohorts. Collected outcomes include the modified Harris Hip Score, Nonarthritic Hip Score, Lower Extremity Functional Scale score, Hip Outcome Score-Activities of Daily Living, Hip Outcome Score-Sports Specific Subscale, 33-item International Hip Outcome Tool score, pain levels, patient satisfaction, and conversion to THA.
Results: In total, 38 patients with GO were 1:1 matched to a MC cohort. The GO cohort had significantly decreased baseline JSW at 50° (P = .002) and greater chondrolabral junction breakdown (P = .037). The GO and MC cohorts achieved similar outcomes for all 6 PROMs, rates of conversion to THA, pain levels, and patient satisfaction. Kaplan-Meier survival analysis demonstrated that the patients experienced a similar overall 18-year THA-free survival rate (GO: 71.1% vs MC: 84.2%; P = .101). To isolate the long-term effects of GO on hip arthroscopy outcomes, 6- to 18-year THA-free survivorship was examined, revealing that the GO cohort (-13.1%) experienced a significantly greater decrease compared with the MC cohort (-5.3%) (P = .008).
Conclusion: Patients with GO had significantly lower baseline ipsilateral JSW at 50° and greater intraoperative severity of chondrolabral junction breakdown. Furthermore, the GO cohort experienced a significantly greater decrease in long-term THA-free survivorship 6 to 18 years after hip arthroscopy.
Keywords: chondrolabral junction; global acetabular overcoverage; hip arthroscopy; long-term survivorship.
Lee JS, Gillinov, SM, Siddiq BS, Dowley KS, Dean MC, Cherian NJ, Eberlin CT, Kucharik MP, Martin SD. Association Between Global Overcoverage and Long-term Survivorship, Chondrolabral Junction Breakdown, and Reduced Joint Space Width: Minimum 8-Year Follow-up. The American Journal of Sports Medicine. 2025 Mar;53(4):900-910. https://doi.org/10.1177/03635465251317738 Online Ahead of Print 19 Feb 2025
Relationship Between Neighborhood-Level Socioeconomic Status and Functional Outcomes After Hip Arthroscopy, Am J Sports Med
Conclusion: Although hip arthroscopy patients experiencing a greater neighborhood-level socioeconomic disadvantage exhibited significantly lower preoperative baseline PROM scores, this disparity resolved at 1-year follow-up. In fact, when adjusting for patient characteristics including ADI score, more disadvantaged patients achieved greater odds of achieving the minimal clinically important difference. The present study is merely a first step toward understanding health inequities among patients seeking orthopaedic care. Further development of clinical guidelines and health policy research is necessary to advance care for patients from disadvantaged communities.
Lee JS, Rachala RR, Gillinov SM, Siddiq BS, Dowley KS, Cherian NJ, Martin SD. Relationship Between Neighborhood-Level Socioeconomic Status and Functional Outcomes After Hip Arthroscopy. Am J Sports Med. 2024 Oct;52(12):3054-3064. https://doi.org/10.1177/03635465241272077 PMID: 39272223
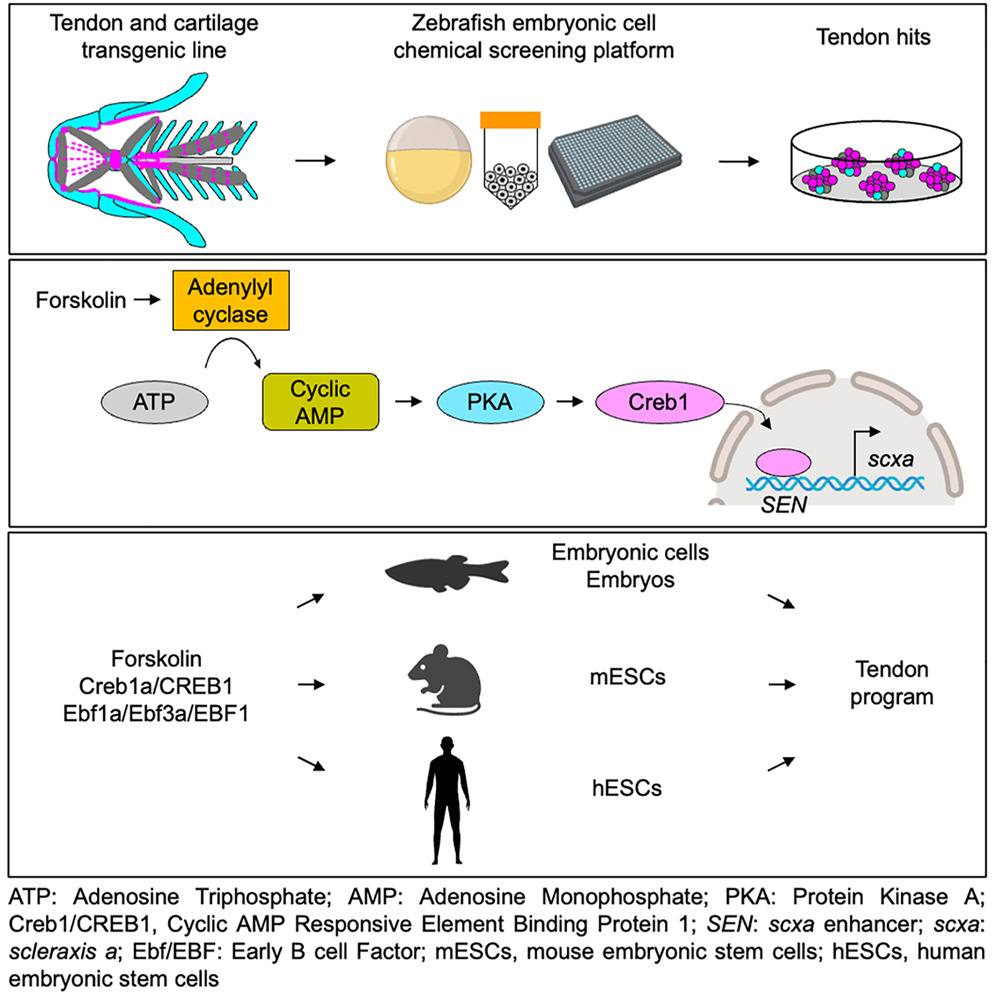
A Conserved Transcription Factor Regulatory Program Promotes Tendon Fate, Developmental Cell
- Chemical screen identifi es the cAMP-PKA-Creb1/CREB1 pathway as promoting tendon fate
- Creb1a induces tendon fate by directly activating the newly identifi ed scxa enhancer SEN
- Motif analysis of enhancer regions identifi es Ebf/EBF as a novel tendon regulator
- Creb1/CREB1 and Ebf/EBF are suffi cient and necessary for tendon development
Niu X, Melendez D, Raj S, Cai J, Senedeera D, Mandelbaum J, Shestopalov IA, Martin SD, Zon LI, Schlaeger TM, Lai LP, McMahon AP, April M. Craft AM, Galloway JL. A Conserved Transcription Factor Regulatory Program Promotes Tendon Fate. Devopmental Cell. https://doi.org/10.1016/j.devcel. Online ahead of print. PMID: 49216481
Hip arthroscopy versus physical therapy for the treatment of symptomatic acetabular labral tears in patients older than 40 years: 24-month results from a randomized controlled trial, Am J Sports Med
Conclusion: In patients ≥40 years of age with limited osteoarthritis, hip arthroscopy with postoperative physical therapy led to better outcomes than PTA at a 24-month follow-up. However, additional preoperative physical therapy did not compromise surgical outcomes and allowed some patients to avoid surgery. When surgery is indicated, age ≥40 years should not be considered an independent contraindication to arthroscopic acetabular labral repair.
Martin SD, Dean MC, Gillinov SM, Cherian NJ, Eberlin CT, Kucharik MP, Abraham PF, Nazal MR, Conaway WK, Quinlan NJ, Alpaugh K, Torabian KA. Hip arthroscopy versus physical therapy for the treatment of symptomatic acetabular labral tears in patients older than 40 years: 24-month results from a randomized controlled trial. Am J Sports Med. 2024 Aug 5:3635465241263595. https://doi.org/10.1177/03635465241263595 Online ahead of print. PMID: 39101607.
Variation in the Cost of Hip Arthroscopy for Labral Pathological Conditions: A Time-Driven Activity-Based Costing Analysis, JBJS
Conclusions: By applying TDABC to outpatient hip arthroscopy, we identified wide patient-to-patient cost variation that was most effectively explained by the method of labral management, the operating surgeon, the osteoplasty type, and the surgery center. Given current procedural coding trends, declining reimbursements, and rising health-care costs, these insights may enable stakeholders to design bundled payment structures that better align reimbursements with costs.
Dean MC, Cherian NJ, Beck da Silva Etges AP, Dowley KS, LaPorte ZL, Torabian KA, Eberlin CT, Best MJ, Martin SD. Variation in the Cost of Hip Arthroscopy for Labral Pathological Conditions: A Time-Driven Activity-Based Costing Analysis. J Bone Joint Surg Am. 2024 Aug 7, 106(15):p 1362-1372. https://doi.org/10.2106/jbjs.23.00500 Epub ahead of print. PMID: 38781316
2024 JBJS Essential Surgical Techniques Subspecialty Procedures Award
Puncture Capsulotomy Technique During Hip Arthroscopy. (Video) Puncture capsulotomy during hip arthroscopy, JBJS Essential Surgical Techniques
Gillinov SM, Siddiq BS, Cherian NJ, Martin SD. Puncture Capsulotomy Technique During Hip Arthroscopy. (Video) Puncture capsulotomy during hip arthroscopy. JBJS Essential Surgical Techniques 14(2):e23.00061, April-June 2024. 10.2106/JBJS.ST.23.00061 PMCID: PMC11186812 PMID: 38903605
Chondrolabral Junction Breakdown Predicts Conversion to Total Hip Arthroplasty After Hip Arthroscopy for Symptomatic Labral Tears: Minimum 8-Year Follow-up, Am J Sports Med
Conclusion: Although most patients achieved favorable minimum 8-year outcomes, several pre- and intraoperative factors were associated with THA conversion; of these, worse CLJ breakdown, higher Tönnis grade, and older age were the strongest predictors.
Dean MC, Cherian NC, LaPorte ZL, Eberlin CT, Wang C, Torabian KA, Dowley KS, Kucharik MP, Abraham PF, Nazal MR, Martin SD. Chondrolabral Junction Breakdown Predicts Conversion to Total Hip Arthroplasty After Hip Arthroscopy for Symptomatic Labral Tears: Minimum 8-Year Follow-up. Am J Sports Med. 2024 Apr; 52(5): 1153–1164. https://doi.org/10.1177/03635465241234258 PMID: 38476016 PMCID: PMC10986152
High Pelvic Incidence Predicts Inferior Outcomes Following Hip Arthroscopy for Femoroacetabular Impingement and Acetabular Labral Tears, Am J Sports Med
Conclusion: After hip arthroscopy, patients with a high PI (>60°) exhibited inferior PROMs, rates of achieving clinically meaningful thresholds, and satisfaction at 12 and 24 months relative to patients with low or moderate PI. Conversely, the outcomes of patients with low PI (<45°) were found to match the trajectory of those with a neutral spinopelvic alignment (45°≤ PI ≤ 60°). These findings highlight the importance of analyzing spinopelvic parameters preoperatively to prognosticate outcomes before hip arthroscopy for acetabular labral tears and FAI.
Torabian KA, Cherian NJ, Eberlin CT, Dean MC, Dowley KS, LaPorte ZL, Kucharik MP, Gillinov SM, Martin, SD. High Pelvic Incidence Predicts Inferior Outcomes Following Hip Arthroscopy for Femoroacetabular Impingement and Acetabular Labral Tears. Am J Sports Med. 2024 Mar;52(3):631-642. https://doi.org/10.1177/03635465231219261 PMID: 38369972 PMCID: PMC10905981
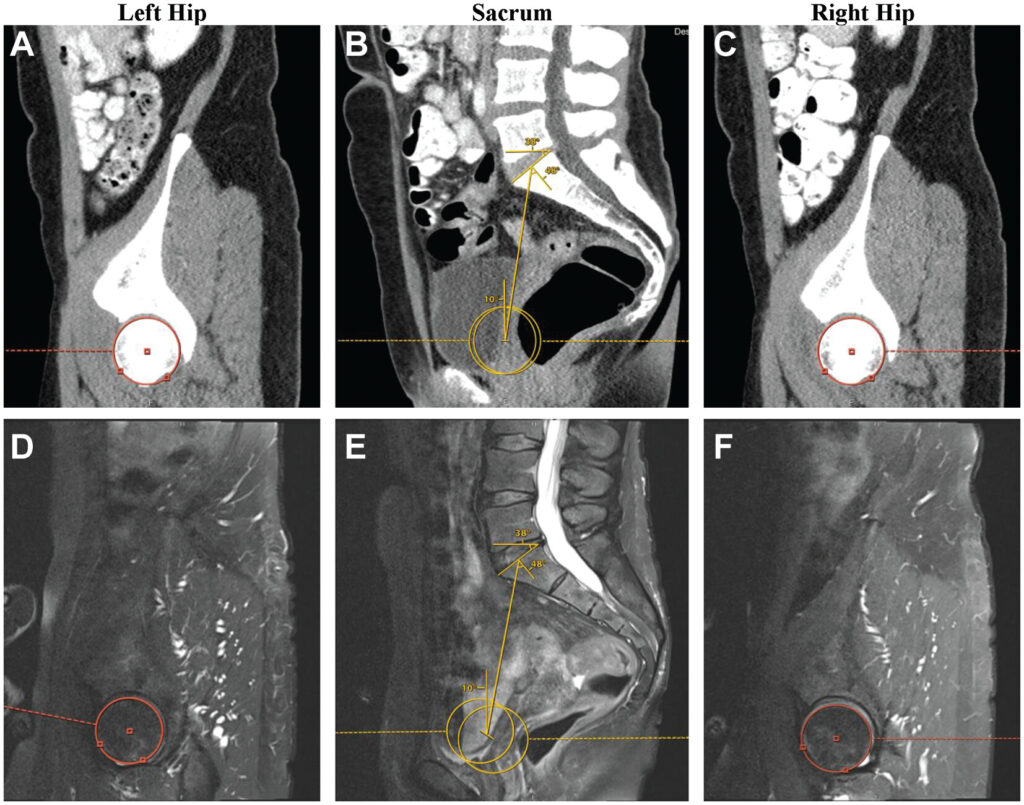
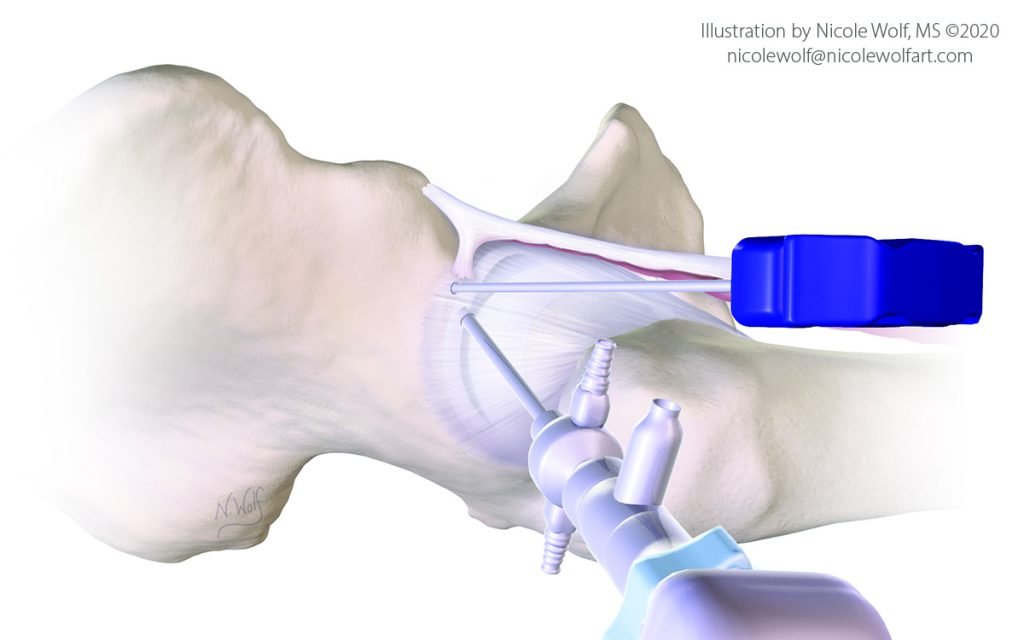
Harvest and Application of Bone Marrow Aspirate Concentrate to Address Acetabular Chondral Damage During Hip Arthroscopy, JBJS Essential Surgical Techniques
Martin SD, Eberlin CT, Kucharik MP, Cherian NJ. Harvest and Application of Bone Marrow Aspirate Concentrate to Address Acetabular Chondral Damage During Hip Arthroscopy. JBJS Essential Surgical Techniques 13(2):e22.00010, April-June 2023. https://doi.org/10.2106/JBJS.ST.22.00010
Comparing the Risk of Osteonecrosis of the Femoral Head Following Intra-articular Corticosteroid and Hyaluronic Acid Injections, JBJS
Conclusions: The incidence of ONFH after intra-articular hip injection was similar between patients who received CSIs and those who received HAIs. Although this study could not determine whether intra-articular injections themselves (regardless of the drug that was used) lead to ONFH, the results suggest that ONFH after CSI often may be due, in part, to the natural course of the underlying disease. Future randomized controlled trials are needed to definitively answer this question; in the interim, clinicians may be reassured that they may continue judicious use of CSIs as clinically indicated.
Varady NH, Abraham PF, Kucharik MP, Freccero DM, Smith EL, Martin SD. Comparing the Risk of Osteonecrosis of the Femoral Head Following Intra-articular Corticosteroid and Hyaluronic Acid Injections. J Bone Joint Surg Am. 2022 Jun 15;104(12):1055-1060. [Published Online Ahead of Print 2022 Mar 11] http://doi.org/10.2106/JBJS.21.01043 PMID: 35275891
Functional Outcomes of Arthroscopic Acetabular Labral Repair with and without Bone Marrow Aspirate Concentrate, JBJS
Conclusions: Patients with moderate cartilage injury undergoing arthroscopic acetabular labral repair with BMAC application reported significantly greater functional improvements when compared with similar patients without BMAC application.
Martin SD, Kucharik MP, Abraham PF, Varady NH, Meek WM, Nazal MR. Functional Outcomes of Arthroscopic Acetabular Labral Repair with and without Bone Marrow Aspirate Concentrate. JBJS. 2022 Jan 5;104(1):4-14. doi.org/10.2106/JBJS.20.01740 PMID: 34648479
Minimum 2-Year Functional Outcomes of Patients Undergoing Capsular Autograft Labral Reconstruction, Am J Sports Med
Conclusions: In this study of 97 hips undergoing arthroscopic labral repair with capsular autograft labral reconstruction, we found favorable outcomes that exceeded the MCID thresholds in the majority of patients at a mean 28.2 months’ follow-up. Future studies should compare outcomes between this technique and other methods of autograft and allograft reconstruction to determine differences in patient-reported outcomes, donor-site morbidity, and complications.
Kucharik MP, Abraham PF, Nazal MR, Varady NH, Meek WM, Martin SD. Minimum 2-Year Functional Outcomes of Patients Undergoing Capsular Autograft Labral Reconstruction. Am J Sports Med. 2021 Aug;49(10):2659-2667. doi.org/10.1177/03635465211026666. Epub 2021 Jul 2. PubMed PMID: 34213975
Hip Arthroscopy versus Physical Therapy for the Treatment of Symptomatic Acetabular Labral Tears in Patients Older than 40: A Randomized Control Trial, Am J Sports Med
Conclusion: In patients older than 40 years with limited osteoarthritis, arthroscopic acetabular labral repair with postoperative physical therapy led to better outcomes than physical therapy alone. Thus, age over 40 years should not be considered a contraindication to arthroscopic acetabular labral repair.
Martin SD, Abraham PF, Varady NH, Nazal MR, Conaway WC, Quinlan NJ, Alpaugh K. Hip Arthroscopy versus Physical Therapy for the Treatment of Symptomatic Acetabular Labral Tears in Patients Older than 40: A Randomized Control Trial. Am J Sports Med. 2021 Apr;49(5):1199-1208. doi.org/10.1177/0363546521990789 Epub 2021 Mar 3. PMID: 33656950
Translational Relevance of the Goat as a Preclinical Model of the Human Labrum and Chondrolabral Junction—Histological Study, J Ortho Res.
Statement of Clinical Significance: Establishment of a large animal model and deeper knowledge of the histological composition of the hip joint will enhance our study of the acetabular labrum, including repair techniques.
Rajappa R, Nazal MR, Stelzer JW, Hsu H, Conaway WK, Rokkappanavar S, Niu W, Upadhyaya S, Alpaugh K, Spector M, Martin SD. Translational Relevance of the Goat as a Preclinical Model of the Human Labrum and Chondrolabral Junction—Histological Study. J Ortho Res. 2020 May 38(5): 1070-80. Published online 2019 2 December. https://doi.org/10.1002/jor.24546
- Unique histology of the chondrolabral junction
- Caprine Model
- Unique type-1, crimped, loose collagen
• Answers the question of how the junction can hold up over time - Junction under huge sheer forces
- Serves as a bridge between fibrocartilage of the hip labrum and articular cartilage of acetbulum
• Leads us on a quest to find Orthobiologics - Current techniques cannot recapitulate the unique histology of the chondrolabral junction

Hip Joint Surgical Technique Videos
Gluteal Tendon Repair Using an Endoscopic Transosseous Equivalent Double Row Repair Technique, JBJS Essential Surgical Techniques
| Mun JS, Gillinov SM, Lee JS, Martin SD. Gluteal Tendon Repair Using an Endoscopic Transosseous Equivalent Double Row Repair Technique. JBJS Essential Surgical Techniques. July-September 2025; 15 (3): e24.00025 https://doi.org/10.2106/JBJS.ST.24.00025 |
Arthroscopic Reconstruction of the Acetabular Labrum Using an Autograft Hip Capsule. (Video) Puncture capsulotomy during hip arthroscopy, JBJS Essential Surgical Techniques
| Siddiq BS, Gillinov SM, Cherian NJ, Martin SD. Arthroscopic Reconstruction of the Acetabular Labrum using Autograft Hip Capsule. (Video) JBJS Essential Surgical Tech. 2024 Oct Dec; 14(4):e23.00068 https://doi.org/10.2106/JBJS.ST.23.00068 PMCID: PMC11617351 PMID: 39650793 |
2024 JBJS Essential Surgical Techniques Subspecialty Procedures Award
Puncture Capsulotomy Technique During Hip Arthroscopy. (Video) Puncture capsulotomy during hip arthroscopy, JBJS Essential Surgical Techniques
Gillinov SM, Siddiq BS, Cherian NJ, Martin SD. Puncture Capsulotomy Technique During Hip Arthroscopy. (Video) Puncture capsulotomy during hip arthroscopy. JBJS Essential Surgical Techniques 14(2):e23.00061, April-June 2024. 10.2106/JBJS.ST.23.00061 PMCID: PMC11186812 PMID: 38903605
Harvest and Application of Bone Marrow Aspirate Concentrate to Address Acetabular Chondral Damage During Hip Arthroscopy, JBJS Essential Surgical Techniques
Martin SD, Eberlin CT, Kucharik MP, Cherian NJ. Harvest and Application of Bone Marrow Aspirate Concentrate to Address Acetabular Chondral Damage During Hip Arthroscopy. JBJS Essential Surgical Techniques 13(2):e22.00010, April-June 2023. https://doi.org/10.2106/JBJS.ST.22.00010
Use of Stem Cells with Arthroscopic Hip Labral Repair
By using BMAC to augment labral repairs and coat chondrolabral junction breakdown, we are able to introduce mesenchymal stem cells to peripheral acetabular tissue with little to no drawbacks, while avoiding donor-site morbidity, open procedures, and multiple surgeries.
Stelzer JW, Martin SD. Use of Bone Marrow Aspirate Concentrate with Acetabular Labral Repair for the Management of Chondrolabral Junction Breakdown. Arthrosc Tech. 2018 Oct; 7(10): e981–e987. Published online 2018 Sep 1. doi:10.1016/j.eats.2018.06.003. PMID:30377577
Puncture Capsulotomy During Hip Arthroscopy for Femoroacetabular Impingement: Preserving Anatomy and Biomechanics
We describe an arthroscopic technique for the treatment of labral pathology and femoroacetabular impingement that provides excellent access to the central and peripheral compartments while preserving the biomechanically crucial components of hip joint stability.
Conaway WK, Martin SD. Puncture Capsulotomy during Hip Arthroscopy for FAI: Preserving Anatomy and Biomechanics. Arthrosc Tech. 2017 Dec; 6(6): e2265–e2269. Published online 2017 Nov 27. doi:10.1016/j.eats.2017.08.036.
“In-Round” Labral Repair After Acetabular Recession Using Intermittent Traction
The prevalence of hip arthroscopy has increased exponentially with the advent of arthroscopic labral repair techniques for femoroacetabular impingement. The goal of arthroscopic labral repair is to re-create the anatomic suction seal of the labrum against the femoral head. This technique re-creates the native anatomy and biomechanics of the hip after acetabular recession and labral repair while decreasing traction time.
Skelley NW, Conaway WK, Martin SD. “In-Round” Labral Repair After Acetabular Recession Utilizing Intermittent Traction. Arthrosc Tech. 2017 Oct; 6(5): e1807–e1813. Published online 2017 Oct 9. doi:10.1016/j.eats.2017.08.036.
Arthroscopic Treatment of Pigmented Villonodular Synovitis of the Hip Using Puncture Capsulotomy
Pigmented villonodular synovitis (PVNS) is a monoarticular, benign tumor arising from the synovium. Although classically treated with open synovectomy, arthroscopic treatment has demonstrated good clinical outcomes.
Nazal MR, Parsa A, Martin SD. Arthroscopic Treatment of Pigmented Villonodular Synovitis (PVNS) of the Hip utilizing Puncture Capsulotomy Arthroscopy Techniques. Arthrosc Tech. 2019 Jun;8(6): e641–e646. Epub 2019 Jun 2. doi: 10.1016/j.eats.2019.02.007